Getting credentialed with UnitedHealthcare (UHC) and their behavioral health arm, Optum, is often the first step therapists take to build a sustainable, insurance-based private practice. With over 50 million members, UHC is a juggernaut in the mental health space, and being an in-network provider can virtually guarantee a consistent influx of local clients.
However, many clinicians find the UHC credentialing process to be one of the more technologically intensive. Written by Jason Roy and reviewed by licensed clinicians, this 2026 roadmap will detail the exact steps you need to take to join the UnitedHealthcare network, manage the Provider Express portal, and avoid the common documentation errors that stall applications for months.
Optum vs. UnitedHealthcare: What’s the Difference?
In the behavioral health world, you will see these names used interchangeably. UnitedHealthcare is the umbrella insurance company, but Optum is the specific administrative subsidiary that manages the mental health provider network and claim processing. For all intent and purposes, “credentialing with UHC” means “applying to the Optum network.”
Essential Prerequisites for 2026
Before you ever login to the UHC application portal, you must have your foundation solidified. If you are missing any of these items, your application will be rejected within 48 hours.
- Type 1 and Type 2 NPI: You must have an individual NPI (Type 1). If you are billing under an LLC or corporation, you will also need a Type 2 NPI. If you haven’t done this yet, read our guide on NPI numbers for therapists.
- Active CAQH ProView Profile: This is non-negotiable. Optum pulls your education and work history directly from CAQH. Your profile must be 100% complete and you must “Authorize” Optum/United Behavioral Health to access it.
- Current Malpractice Insurance: Your face sheet must show your name, practice address, and adequate coverage limits (typically $1M/$3M).
- Work History Gaps: Optum requires an explanation for any work history gap exceeding 6 months in the last 5 years.
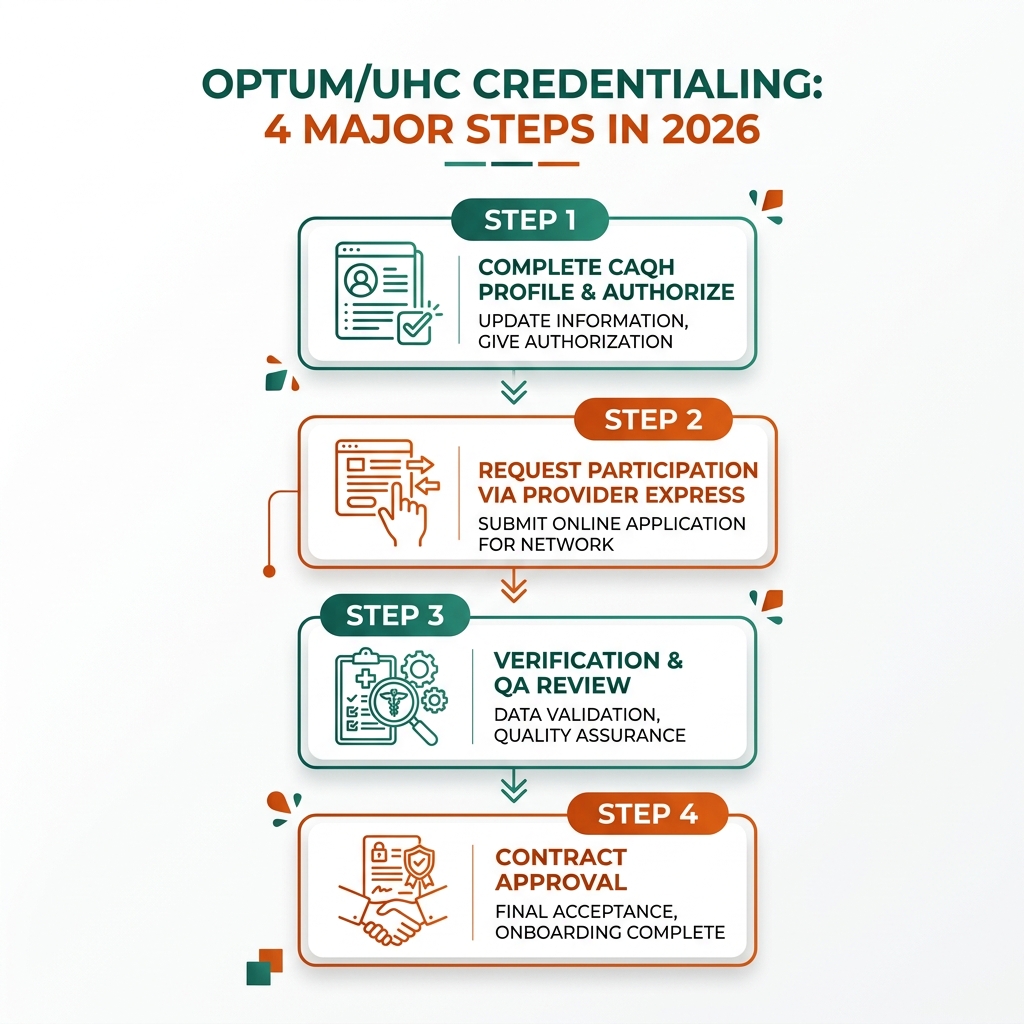
Step-by-Step UHC Credentialing Process
Step 1: The Provider Express Invitation
The gateway to UnitedHealthcare is the Provider Express website. You start by filling out an “Initial Participation Request.” Optum will then review your info and the “Network Need” in your area. If they have a gap for your specialization, they will send an invitation to complete the full application.
Step 2: CAQH Syncing and Attestation
Once invited, you don’t actually “write” a new application; instead, you tell Optum to pull your data from CAQH. Crucial tip: Re-attest your CAQH profile the same day you submit your UHC request. If your CAQH attestation is older than 90 days, the sync may fail, causing a 2-week delay.
Step 3: Primary Source Verification
Optum will verify your state license, your degree-granting institution, and your malpractice history. Unlike other payers, UHC is very strict about board certifications and ensuring your license has zero history of disciplinary action. If they find a discrepancy, they will reach out via the Provider Express portal.
Step 4: The Credentialing Committee Board
After verification, your packet goes to the committee. They meet on a rolling basis to officially vote providers into the network. This is the stage where most of the “waiting” occurs. Use the “Initial Credentialing Status” tool in the portal once a week to monitor progress.
Common Delays and How to Avoid Them
1. Unsigned or Outdated W-9
When you reach the contracting phase, Optum will generate a contract based on your W-9. If the name on your W-9 doesn’t match your NPI registry or your tax ID record exactly, the system will kick the contract back. Ensure your business name matches your state filing precisely.
2. Practice Address Documentation
Optum does not accept P.O. boxes for service locations. If you work via telehealth, you must use a physical address where you are located during sessions. If you are starting a private practice in New York, ensure your physical office address is listed first.
Reimbursement and Negotiation
UHC/Optum reimbursement rates for Master’s-level clinicians are generally competitive compared to smaller carriers but often trail behind companies like Blue Cross Blue Shield. Negotiation is possible for solo practitioners only if they can prove a “specialized niche” or a “geographic hardship” in the area.
Many therapists choosing between Alma vs Headway find that these platforms offer slightly higher UHC rates than independent contracts because of their bulk-negotiation power. However, being directly credentialed allows you to hold your own contract and negotiate your specific rates long-term as your practice grows.
What Happens After You’re credentialed?
Once you receive your “Effective Date” letter, you are officially in-network. You will need to setup Optum Pay (their electronic payment portal) to receive direct deposits. You should also ensure you are familiar with proper CPT and ICD-10 coding to ensure your first batch of claims is processed correctly.
The administrative burden of billing and follow-ups can quickly consume 10–15 hours of your week. This is why more and more therapists are moving to full-service partners who handle everything from the initial CAQH sync to the final unpaid claim resolution.
Exclusive Provider Bundle:
Billing + Free Growth
- Professional Medical Billing
- FREE Insurance Credentialing (UHC, BCBS, Aetna)
- FREE TherapyDial Profile Listing
- Priority Practice Support
Stop fighting with Provider Express and CAQH. We handle your complete credentialing and ongoing billing.
HIPAA Compliant & Expertly Managed.
Frequently Asked Questions
1. How long does UnitedHealthcare credentialing take in 2026?
On average, the process takes between 60 and 90 days. However, delays are common if your CAQH profile is not up-to-date or if Optum requires additional documentation for work history gaps over 6 months.
2. Does UHC require a physical office for credentialing?
Yes. Even for telehealth-only practices, UHC/Optum requires a physical address where the clinician is located. They do not accept P.O. boxes as a primary practice location for credentialing.
3. What is Optum Pay?
Optum Pay (formerly EPS) is the electronic payment platform that UnitedHealthcare uses to issue reimbursements to providers. It is a separate registration process that you should complete as soon as you are credentialed to receive direct deposits.
4. Why was my application to the Optum network denied?
Common reasons for denial include “network adequacy,” meaning there are already enough providers of your specialty in your zip code. Other reasons include licensure issues or failure to respond to additional info requests within their 10-day window.
5. Can I see UHC patients while my application is pending?
No. You can only bill as an in-network provider for dates of service occurring on or after your official “Effective Date” provided in your approval letter. Sessions held prior to that date must be billed as out-of-network.